I have to say, having Eva by caesarean was a thoroughly pleasant experience. A couple of weeks before she was born we decided that Eva would be coming out via the sunroof so that gave us time to do a bit of planning. I had two big concerns – controlling my diabetes during and after the op, and making sure Eva didn’t go hypo once she was born. So we did a bit of reading, and decided there were three things we wanted to happen:
Controlling diabetes during a c-section
I wanted to maintain control of my diabetes throughout rather than go on a sliding scale, so we had a chat with the anaesthetist who’d be doing my op. He had his own views on how I should manage my diabetes, but we didn’t agree with them. He wanted me to aim to go into theatre at around 7 or 8, which was fine by me. He suggested I achieve this by reducing my basal to 80% the night before and then to 0% as I went into theatre to avoid going hypo once the baby was born.
I agreed with what he was trying to do – it made perfect sense to play safe and aim to be around 8 for the op. High enough to avoid hypos, but low enough not to cause the baby to mass produce insulin in response to the amount of glucose she’s getting from me and then end up low when that glucose supply stops at birth. I was also just as scared as he was of a post birth hypo – once the placenta has been delivered all those hormones that have been causing insulin resistance for months suddenly disappear, and insulin requirements return to pre pregnancy levels almost immediately.
But I didn’t think his plan would work. So, I explained my plan to him. I’d run at normal basal rates the night before the op, because the stress of knowing I was having a baby in the morning would keep me plenty high enough without reducing basal rates. I’d also monitor it closely through the night and correct if required. I was nil by mouth but we agreed I could use Hypostop gel to treat lows if needed. To avoid the post birth crash, I’d reduce my basal rates to pre pregnancy levels 2 hours before the c-section started, meaning that by the time they got the placenta out, I’d have the right levels of insulin in my system.
He agreed, and it worked. I entered theatre as an 8 and left as a 7, staying around a 7 for the next few hours. He came to visit me the next day to double check what I’d done because he wants to adopt that as his diabetic plan from now on. Isn’t it nice when a doctor actually listens?
Preventing post-birth lows
I controlled my sugars throughout delivery to try and prevent any post birth lows, but I was conscious that there was no guarantee that would work, and anyway, 8 is still higher than a non diabetic woman would run at so there was still some risk of hypos to the baby. For that reason I decided to express colostrum in the week prior to birth, so that we’d have food available for Eva as soon as she was born, without having to resort to formula.
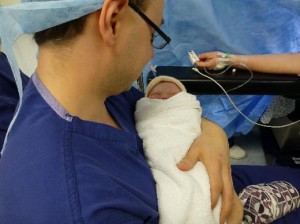
Daddy has a first cuddle before feeding Eva some colostrum while Mummy’s being stitched back together
So we headed into theatre with several tiny syringes filled with less than a teaspoon each of colostrum. We explained to the midwife that if the baby needed food before I could breastfeed we’d like her to have this rather than formula. The midwife said regardless of blood sugar, she’d recommend we give the baby the colostrum anyway, so she could have food as soon as possible. That seemed sensible, so as soon as Eva was born and handed to Geoff, the midwife helped him give Eva her first feed of breastmilk via a syringe. They were putting me back together for the next half hour so I couldn’t feed Eva, but it meant she got some decent food straight away even though her blood sugars were fine. As soon as I was stitched up, they handed her to me and she started feeding within 5 minutes. It worked a treat – we were both relaxed because I wasn’t panicking that she’d has no food and could go low and she wasn’t starving hungry.
When to cut the cord
The final request we had was for the surgeon to delay cutting the umbilical cord until it had stopped pulsating. Practice ;

Congratulations! A fab plan, well executed by helpful medics (for a change!) and managed perfectly by you!
I had a sun-roof job for my son 9 years ago, I couldn’t plan as much as you did, as he was an emergency at 32 weeks, and I was virtually unconscious by the time he arrived (pesky HELLP syndrome and pre-eclampsia)
You’ve given Eva a brilliant start to life, and I’m sure you’ll continue to be a Yummy Mummy for quite some time yet..! Enjoy every moment – life will never be the same, but in the best possible way. Xxx
Alison, I haven’t yet said a big congratulations to you all but just wanted to say you did the whole thing amazingly. Am so glad the section went well, as I believe I’ve already said, it’s a brilliant way to give birth ( but then I haven’t been through the alternative ). I’ve just come back from this year’s brilliant Animas weekend for Sporty type 1’s and discussed giving birth as a type 1 with some girls in their early 20’s. They were concerned that they’d been told to have their babies by 25 but I told them I’d given birth the first time at 34 but that good HBa1c was essential and perhaps aim for 30 years ish to be on the safe side if possible. I’ve also pointed them on to the Shoot up site as a good example of what needs to be done.
I hope you are coping with the post birth lows which I do remember causing me problems but I didn’t have a pump then. Anyway, hooray for you and Eva.